
Revenue cycle management is not just about submitting claims. It’s about ensuring that every step, from credentialing to payment posting, works together without breakdowns.
Credifide provides revenue cycle management services designed to reduce friction, prevent avoidable errors, and create predictable reimbursement for healthcare providers. Our focus is on building stable billing operations that hold up under real-world complexity.

Most RCM issues do not start with billing. They begin earlier, with incomplete credentialing, outdated payer information, or inconsistent data across systems.
When revenue cycle management is handled internally, providers often rely on manual workflows, disconnected tools, and reactive problem-solving. Issues surface only after claims are denied, payments are delayed, or balances accumulate.
Even when RCM is outsourced, many providers experience limited visibility into what’s happening behind the scenes. Problems are addressed after they impact revenue rather than being prevented upfront.
These breakdowns are not isolated mistakes. They are symptoms of systems that were never designed to catch issues early.

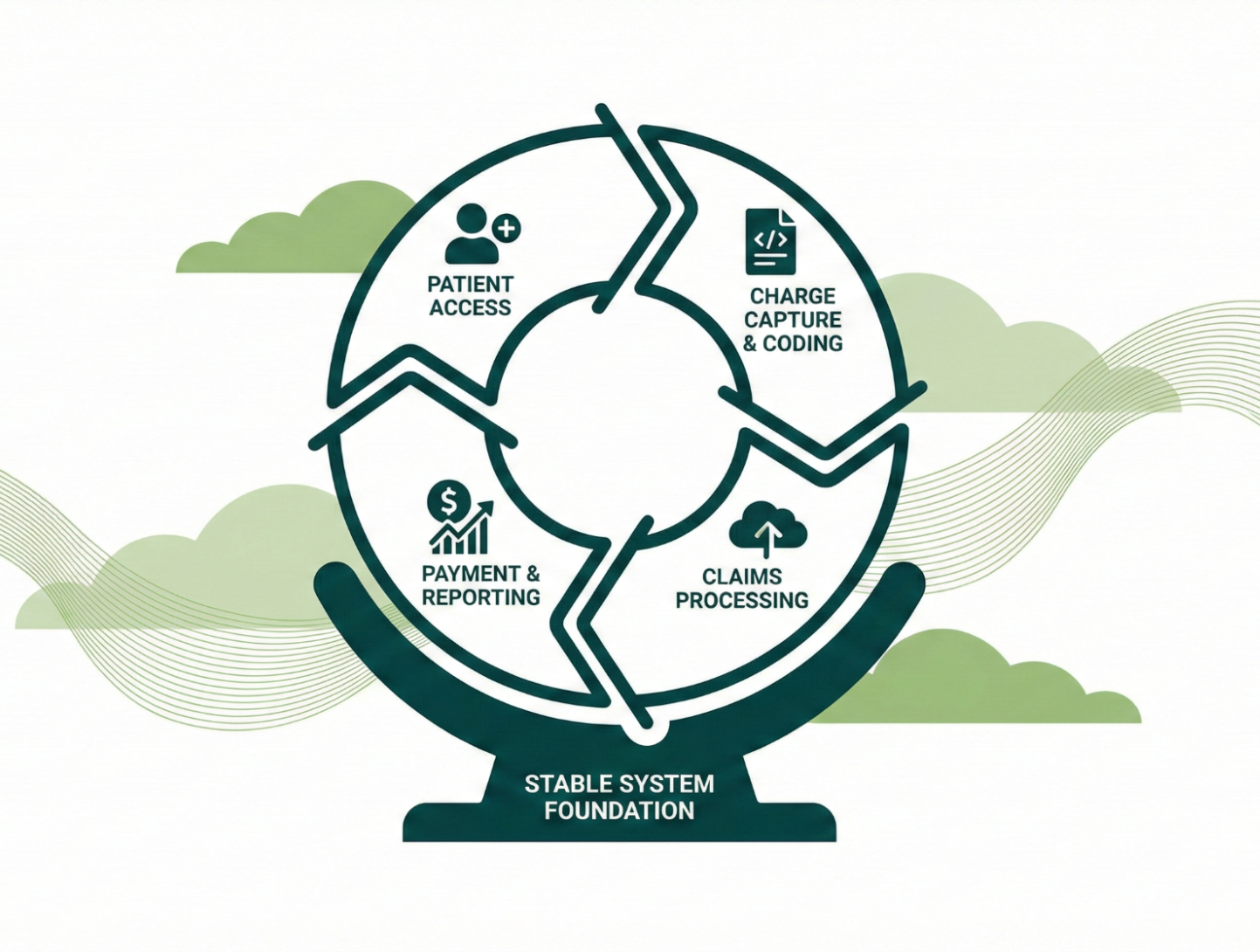

Credifide approaches RCM as a continuous operational system, not a series of disconnected tasks. Our workflows are designed to anticipate issues, validate data, and maintain alignment between credentialing, contracting, and billing.
We use intelligent automation to standardize processes and reduce manual intervention where it introduces risk. At the same time, experienced billing and RCM professionals oversee every workflow to ensure payer rules, regulatory requirements, and provider-specific nuances are applied correctly.
This balance allows us to improve accuracy without losing accountability.
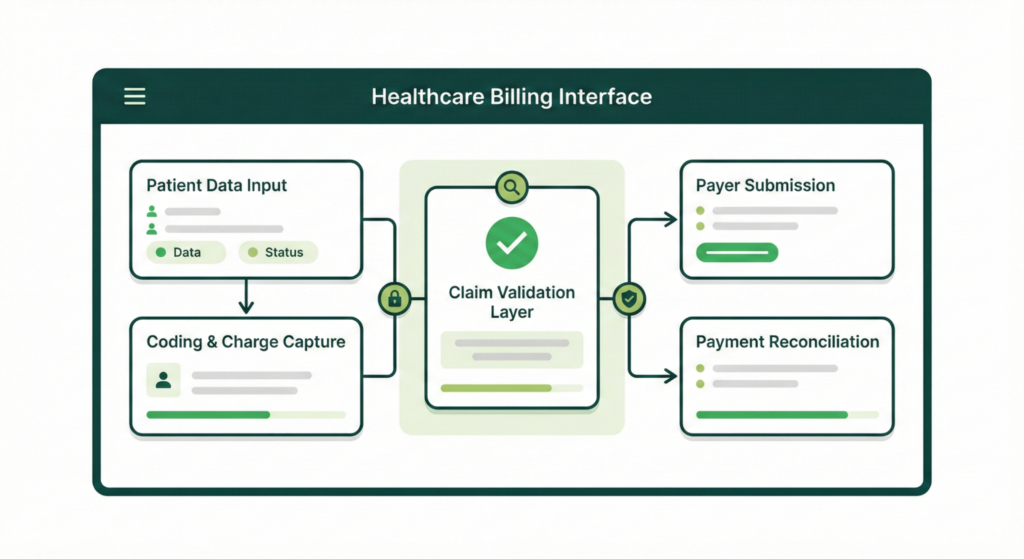
Credifide’s revenue cycle management services cover the full billing lifecycle, from claim creation to reconciliation. Our work is focused on maintaining clean claims, reducing denials, and improving payment consistency over time.
Rather than treating denials as an unavoidable cost of doing business, we analyze patterns, identify root causes, and adjust workflows to prevent repeat issues.



Credifide uses advanced technology to reduce risk before claims are submitted. AI-assisted checks help identify missing or inconsistent data, while rules-based billing logic aligns claims with payer-specific requirements.
Our systems continuously monitor claim status, flag exceptions early, and support faster resolution when issues arise. By identifying patterns across claims and payers, we address systemic issues rather than individual symptoms.
Technology helps us work smarter. Governance ensures we work correctly.
A common frustration with RCM services is not knowing why payments are delayed or where issues originate. Credifide eliminates that uncertainty through built-in transparency.
Providers have visibility into claim status, denial trends, and resolution progress. Communication is proactive, and explanations are clear. You don’t have to chase updates or piece together information from multiple sources.



As practices grow, billing complexity increases. New providers, additional payers, and evolving regulations add layers of risk.
Credifide’s RCM workflows are designed to scale without losing consistency or control. Whether supporting a single provider or a multi-provider organization, our approach remains structured, reliable, and adaptable.


Partner with Credifide for AI-powered provider credentialing, insurance contracting, and RCM built for healthcare professionals.