
Insurance Credentialing is one of the most critical and least forgiving parts of healthcare operations. A single missed detail can delay approvals, disrupt patient access, or prevent reimbursement entirely.
Credifide provides Insurance Credentialing services designed to work reliably over time. We help healthcare providers get credentialed accurately and stay credentialed without interruptions, rework, or unnecessary delays.

For many providers, credentialing becomes difficult not because requirements are unclear, but because the process is fragmented. Information is entered repeatedly across payer portals, documents live in multiple places, and follow-ups depend on manual tracking.
Over time, this leads to stalled applications, missed recredentialing deadlines, and limited visibility into what has actually been completed. Even when credentialing is outsourced, providers are often left waiting for updates or discovering problems only after approvals fail.
These challenges are systemic. They are the result of processes that were never designed to scale or adapt.



Credifide treats Insurance Credentialing as operational infrastructure, not administrative paperwork. Every credentialing workflow is structured, monitored, and governed from start to finish.
We use automated workflows to guide each provider through payer-specific requirements while applying validation checks before submissions occur. This reduces preventable errors and minimizes back-and-forth with payers.
Human expertise remains central to the process. Experienced credentialing specialists oversee each account to ensure accuracy, compliance, and appropriate escalation when needed.
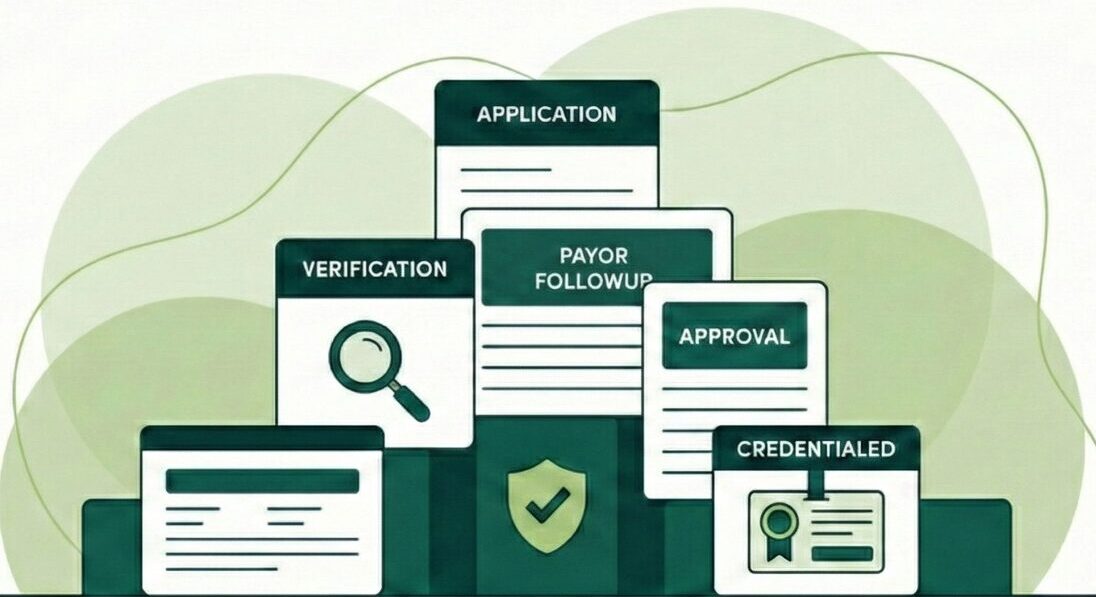
Our insurance Credentialing services support both initial enrollment and long-term maintenance. This includes managing provider data, coordinating payer submissions, monitoring application status, and maintaining credentialing records over time.
Rather than treating credentialing as a one-time task, we design processes that support ongoing compliance as providers, payers, and regulations change.

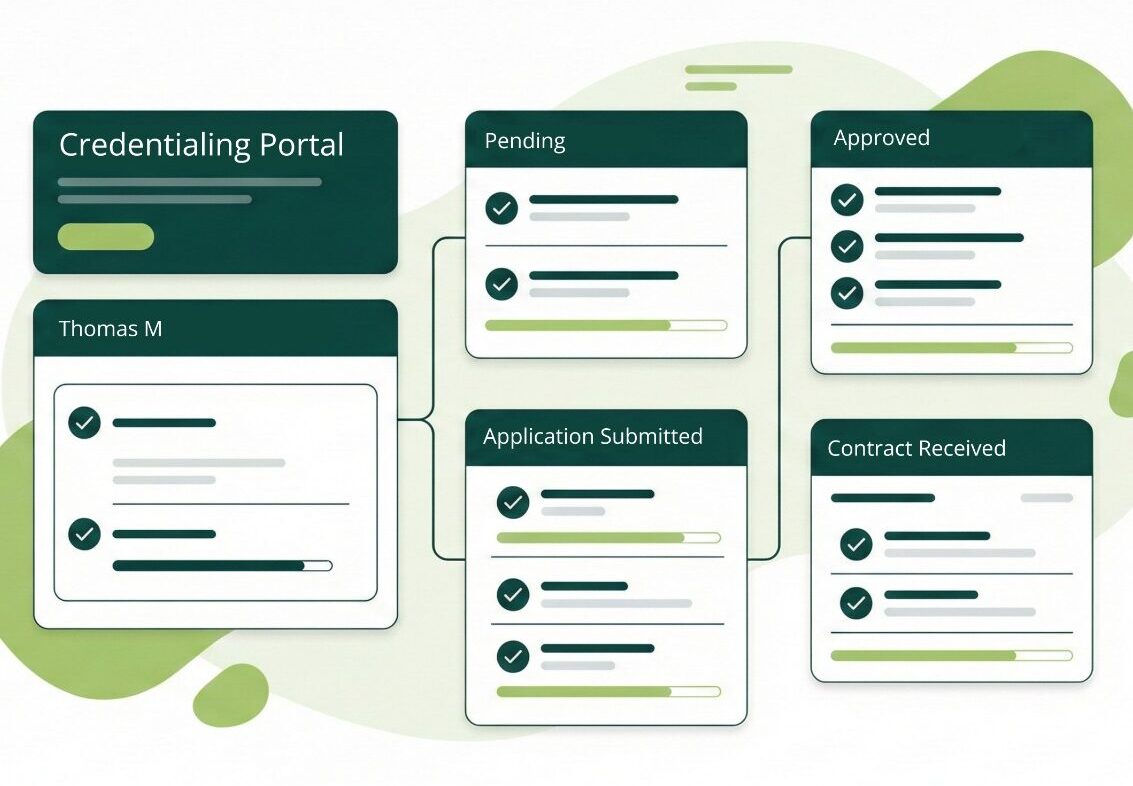

Credifide uses technology where it meaningfully reduces risk. Automation handles repetition and tracking, while AI-assisted validation helps identify inconsistencies before they delay approvals.
Our systems continuously monitor deadlines, flag missing or conflicting information, and maintain centralized records that are audit-ready. This allows issues to be addressed early, rather than after they impact participation or billing.
Technology improves consistency. Oversight ensures correctness.
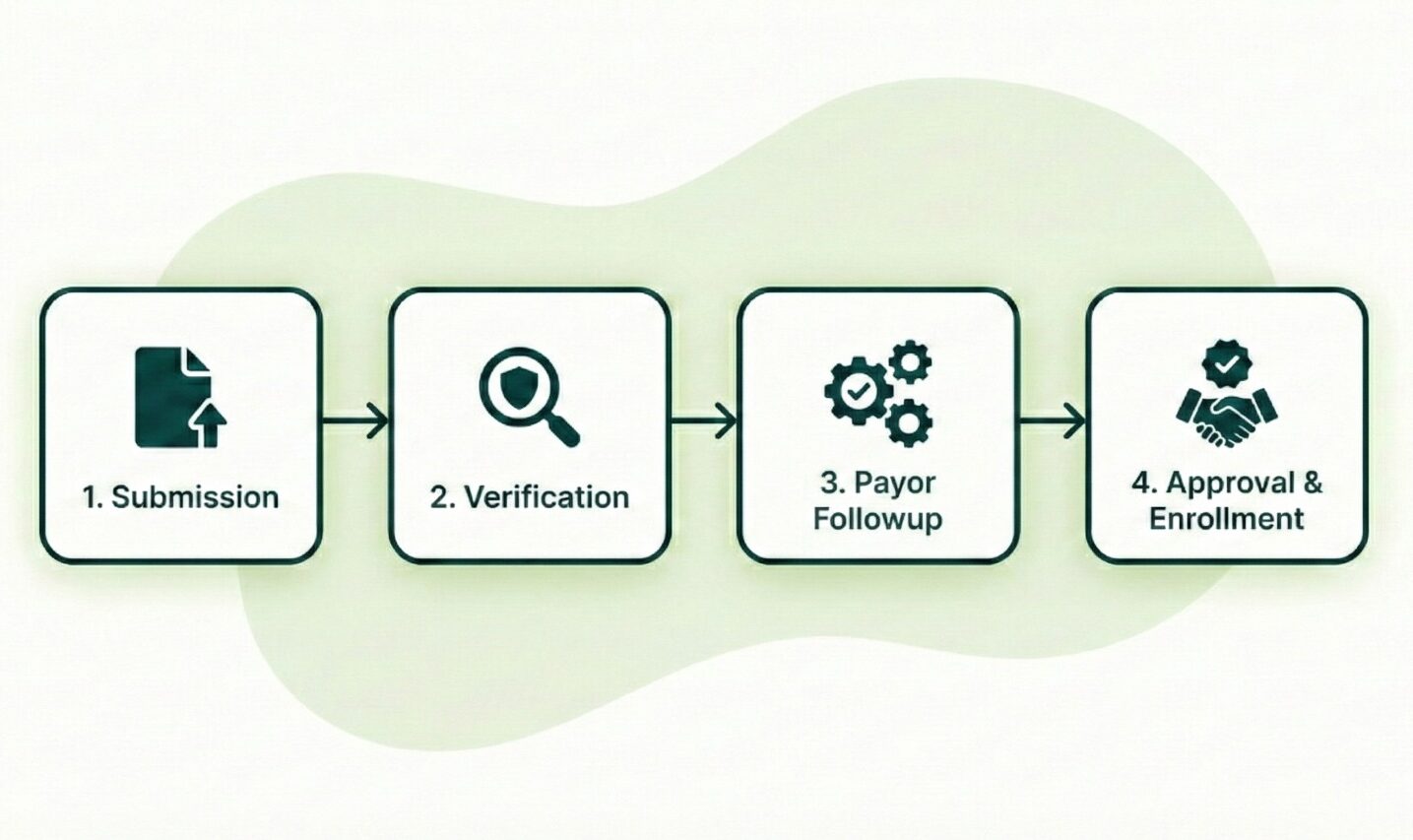
Credentialing should never feel opaque. At Credifide, transparency is part of the process, not an afterthought.
Providers have clear visibility into where applications stand, what has been completed, and what remains pending. Updates are proactive, and documentation is accessible when needed. You are never left guessing or chasing information.



As practices grow, credentialing becomes more complex. Multi-provider groups, multi-state licensure, and expanding payer relationships introduce new variables and risk.
Credifide’s credentialing workflows are designed to scale without losing control. Whether supporting a single provider or a growing organization, our approach remains structured, consistent, and dependable.

Credifide is built for healthcare providers who want credentialing done correctly, transparently, and without disruption to clinical operations.
We don’t rely on shortcuts or reactive fixes. We design systems that work.

Partner with Credifide for AI-powered provider credentialing, insurance contracting, and RCM built for healthcare professionals.